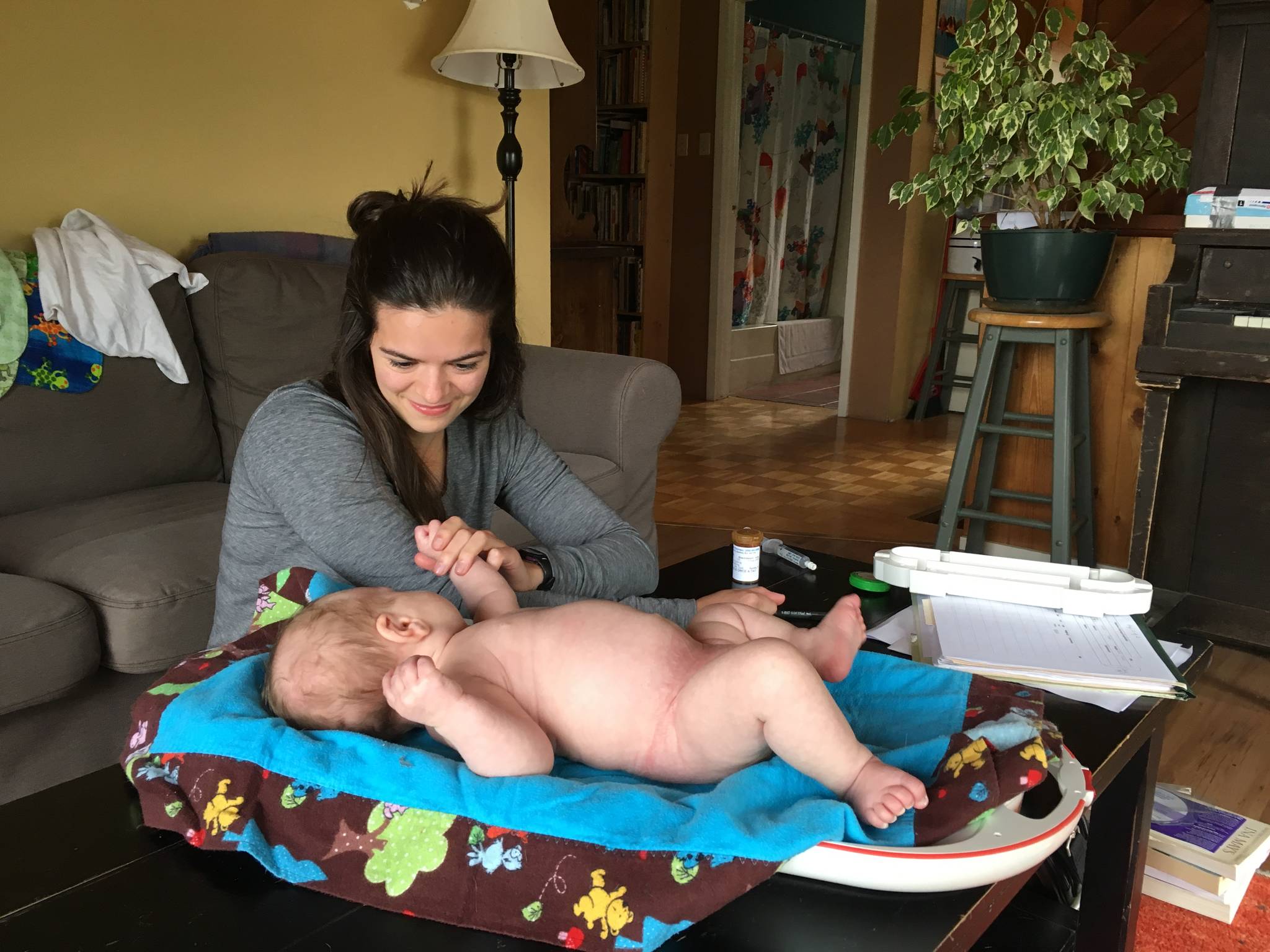
Northern B.C. mother Lauren Fraychineaud was born at home with the help of a midwife. And from the start of her own first pregnancy, she vowed to do the same for her babies. Even if she had to travel from her home in Terrace to Smithers, while in labour, to do it.
“We wanted to have a homebirth, which is not an option in Terrace, so we had to go to Smithers,” said Fraychineaud as she balanced her then 8-month-old daughter, Cea, on her lap.
“Which isn’t really the same option. It’s not my home… staying in my home wouldn’t have included packing up all my stuff up and having to leave.”
Currently, midwives hold privileges in a number of communities in the region, including Prince George, Smithers, Dawson Creek, Hazelton, Village of Queen Charlotte and Masset. But there is a gap in service in the Skeena coast area of northern B.C., leaving expectant mothers who want the option of a midwife no choice but to travel hours outside of their community to get it.
But the decision to travel meant having the ability to choose how Fraychineaud’s maternity care would look. She felt there was more of a continuum of care with midwifery, as the same care provider would see her throughout her pregnancy, birth and six weeks postpartum.
“It’s a different model of care. Generally, it’s about informed choice versus informed consent, which I am a believer of. You’re viewed more as part of a decision-making team versus just being someone whose decisions are made for you.”
According to the BC Midwives Association (MABC), women receiving care from midwives have a lower rate of preterm births, a lower rate of c-sections, are less likely to require obstetrical interventions and require less time in hospital. But not everyone may be willing to travel hours outside of their communities for the option.
“For four to six weeks…they’re away from their support system. Often times they’re having to leave young children in the care of other relatives. The level of stress that produces in the mother… and we know that stress affects outcome… it’s huge,” said Ganga Jolicoeur, CEO of MABC.
“Stressed mom creates a stressed delivery or a stressed baby, and there’s a kind of domino effect.”
For the past two decades, midwives have been legally registered and regulated in B.C. by the College of Midwives of British Columbia. Midwives must complete a four-year degree and go through a similar vetting process as new physicians and obstetricians at hospitals to gain rights to provide in-hospital births.
READ MORE: Midwives celebrate 20 years in B.C.
The costs of midwifery services are covered through the province’s Medical Services Plan (MSP).
When Fraychineaud became pregnant, she sought the services of the midwife closest to her — Angela Smith, who has been a registered midwife for five years out of Hazelton. She agreed to travel the 300-kilometre round trip distance to see Fraychineaud every month for the first 28 weeks of her pregnancy. The visits increased to a weekly basis as her due date approached.
“Same as what you’d do in a prenatal clinic, but you don’t have to go to her. She comes to you,” Fraychineaud said.
In case of complications, Fraychineaud was required to give birth close to a hospital where Smith also held rights to work. This meant Fraychineaud’s idea of a homebirth involved renting a house in Smithers, where the maternity ward at the hospital there is equipped to provide surgical backup if needed.
When the labour pains started, Fraychineaud and her husband packed their bags and prepared for the two-hour drive to Smithers.
“We went right away because we didn’t want to be travelling while I was in really active labour,” Fraychineaud said. “It was less than ideal, but better than nothing.”
As her labour extended past 20 hours, she was transferred to the Smithers hospital for a Cesarean, where she said Smith stayed involved throughout the process, working closely with the surgeon as part of a team.
“A big concern for us was having our care get turned over and switching hands, which I didn’t want… and that didn’t happen at all. She was involved and she was in with a c-section for us and took care of Flint [the baby]. He came out right away,” she said.
Bringing midwifery to Terrace
One registered midwife is currently providing prenatal and postpartum care to mothers in Terrace, Kitimat and the Nass Valley but she needs to go through the accreditation process with Northern Health first to gain rights to work at Mills Memorial Hospital.
This is important, considering an average of 70 per cent of births attended by midwives occur in hospitals, according to MABC. Until then, Katherine Puchala out of Matrum Midwifery can’t deliver babies at home or in hospital, but has been driving to her clients to provide care since March.
She primarily focusses on postpartum care, but when prenatal care is needed she makes sure to let the families know that care will be transferred to the physician group when it comes time to deliver.
“Some families wish to be transferred earlier so they may get to know the various doctors who might be there for their birth and others wish to retain midwifery care longer,” Puchala wrote in an email to the Terrace Standard.
Service for Terrace would not only help keep mothers closer to home, but it could also provide more access to maternity care services in rural B.C., according to Ganga Jolicoeur, CEO of the Midwives Association of BC (MABC).
READ MORE: Community must demand midwifery for itself
“There are gaps, right? One-sixth of BC residents are not attached to a primary care provider — they’re not attached to a family doctor,” she said. “There are fewer physicians able to provide maternity care services because they’re also so busy with the rest of the life cycle. Midwifery can really help address where those gaps are.”
In 2014, the MABC announced that it wants to increase the number of births by midwife in the province to 35 per cent by 2020. The idea is to have more access to maternity services in rural and northern communities, improve health outcomes for women and newborns and reduce health care costs.
Northern Health’s regional chief medical officer Dr. Jaco Fourie said the health authority is supportive of midwifery care, and conversations have been held between Puchala, the current general practitioner obstetrical group and a gynecologist on how the service would work here.
The midwife would then start the process of gaining privileges at the hospital through the health authority’s Medical Staff Bylaw, whose process includes obtaining relevant documentation from the province’s licensing and regulatory bodies. The BC College of Midwives (CMBC), he said, is currently working through concluding a process with the midwife before they can move forward.
Doris Chan, CMBC deputy registrar and director of finance, was unable to comment on a particular midwife’s situation due to privacy policies.
But when the process does conclude, Fourie said the accreditation process should move quickly. “The moment we get the green light, our paperwork is already done. I’ve already signed off on it in principle. If we get a green light from the College of Midwives then all we do is we provide this to our credentialing committee. From the time they’ve given the green light till she’s able to practice usually takes about 72 hours.”
If the Terrace midwife does obtain hospital credentials and opens a clinic, she’ll most likely need another midwife to work alongside her to rotate on-call responsibilities as a shared-team. Usually, midwives work in groups of two or three, according to MABC, but they may work as solo providers or in interdisciplinary teams as well.
Fourie said there are no current efforts on Northern Health’s end to recruit more midwives to Terrace, but if more midwives want to start their practices here, he said they are welcome to follow the same privileging process as any other new physician.
“If another midwife comes in the interim and wants to start working, there are no barriers other than there has to be a discussion with the existing care delivery group of what the service delivery model is going to look like,” Fourie said.
Across the north, the health authority is reviewing how midwifery can work in a more integrated model with maternity services, specifically by looking into how they can better support recruitment and streamline the process of bringing more midwives into the hospital setting.
Safer delivery for rural mothers
There is medical reasoning why some mothers should not travel for any reason close to their delivery date. According to a 2011 study published by University of British Columbia rural health researcher Dr. Jude Kornelsen and colleagues, infant mortality rates are three times higher for women who travel more than four hours to deliver. There was also a higher rate of preterm births and babies with low birth weights for women who drove more than two hours.
Regardless, according to a 2013 analysis published by the Canadian Institute for Health Information, 40 per cent of women living in rural Canada drive more than an hour to give birth, 17 per cent driving more than two hours.
If midwifery services are able to come to Terrace, an expectant mother in Prince Rupert said it would also give her the ability to choose how she wanted her care to look.
“I found out I was pregnant and started looking into my options and found out there really wasn’t any,” Ashley Hunt said over the phone.
Because it’s more important for her to stay close to home, she said she won’t be travelling to Hazelton for midwifery care and will deliver in hospital instead.
“I basically have no choice but to give birth in a hospital with the care of a nurse and a doctor,” she said. “There was no choice to have a homebirth or a midwife or a birth centre, none of those.”
A petition titled Support for Midwifery in Terrace, BC was created in July by local doula Andrea Eastman. It called for more support from Northern Health to bring midwifery services to the city. To date, it has received 661 signatures.
READ MORE: Bring midwifery to Terrace
“It will happen,” Fourie said. “It’s beyond the ‘let’s talk about it’ stage, it’s about okay, there will be a review and that’s been already postulated, the person that will be responsible for this will be the medical lead of obstetrical services of Northern Health and Northern Health project managers,” said Fourie. “How to integrate, not should we integrate — how do we integrate midwifery into our practices?”
Jolicoeur agreed collaboration between midwives and other health professionals is key, and feels positive about conversations held so far about expanding services in northern B.C.
“A lot of our midwives have done that legwork themselves, but we certainly have been invited in and it’s been really positive,” she said. “I’m super optimistic about the expansion of midwifery services in Northern Health.”
While it’s unclear where the process now stands now, Fraychineaud said she plans to continue growing her family and hopes her next delivery can take place in her actual home in Terrace.
“We do plan on having a third child, and it would be nice to have that option… and not have to travel for it — which we will again if we need to.”
Â
brittany@terracestandard.com
Like us on Facebook and follow us on Twitter